On this World Health Day, we call for urgent action to realise...
5 April 2022
By Dr. Mohammed Abdulaziz, Maziko Matemba, Dr. Herilinda Temba and Dr. John Wanyungu
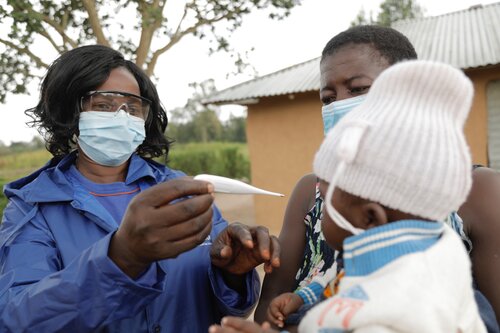
Long before the COVID pandemic threw community health workers (CHWs) into the spotlight, they have been the nucleus of disease control and prevention in sub-Saharan Africa. Given CHWs’ unwavering dedication to saving lives and improving their neighbors’ health, it is a disservice to all Africans that most of these workers remain unpaid, uninsured, and inadequately trained and equipped. From local and national measures formalizing CHWs to a new community health unit being formed within Africa Centre for Disease Control and Prevention (Africa CDC), we are making important moves to elevate CHWs. It is the only way forward if we don’t want to squander the most powerful force we have for achieving universal health coverage (UHC).
As of 2019, half the world’s population lacked access to essential health services, according to the World Health Organization, which concluded that UHC was not possible under the status quo. With CHWs’ reach and their ability to deliver a wide range of preventive, promotive, and curative services, robust integrated CHW programs are indispensable to widening health coverage. And as Ebola and COVID-19 have so starkly shown, infection control doesn’t happen top-down; CHWs are ideally placed to quickly detect, monitor, and halt outbreaks. In fact, the evidence repeatedly shows that both health security and UHC requires investments in the foundations of health systems including well-trained CHWs and other health workers.
Africa CDC leveraged this special role of community health workers with the PACT program, under which CHWs visited over two million households in 27 countries for contact-tracing and other preventive activities. Building on PACT’s success in line with the African Union’s initiative to train and deploy two million CHWs, Africa CDC is establishing a community health unit, and drawing up a community health strategy for 2022-26. Consider Africa CDC’s mission: To strengthen the capacity of public health institutions to detect, prevent, control, and respond to disease threats. It’s clearer than ever that CHWs are integral to that outcome; investing in community health is a regional priority.
Laws cementing CHWs’ status are a critical step. Some county governments in Kenya have recently passed legislation formally recognizing CHWs and giving them a stipend, as well as providing for mentoring and supervision. Kenya’s County Assembly Community Health Services Acts form a legal basis to mobilize domestic resources for community health systems. This embeds in county law the effective delivery of integrated, comprehensive, and quality health services at the local level. Across Kenya, where healthcare delivery has been decentralized to county governments since 2013, most counties are working on community health services bills, as is the national government.
It’s not surprising that communities themselves are leading the charge for these laws. They know the value of CHWs. In Kenya, a coalition known as CHU4UHC (Community Health Units for Universal Health Coverage) emerged last year as local organizations made the case for greater community health worker engagement in the pandemic response. The group broadened its scope to focus on community health service delivery and to advocate for formal recognition of CHWs.
CHW training is the focus of a new strategy in Malawi, where the Health Ministry has launched a one-year CHW certification course to be taught at medical college. While the country has long supported CHWs in important ways, to date, quality of care has suffered from minimal supervision and training and lack of a clear career path. Under the new program, CHWs—who comprise more than half of Malawi’s health workforce—will also receive mentoring and opportunities for career growth.
Malawi recognizes that better trained CHWs will not only improve quality of care but also cut health expenditures in the long term.
Legal frameworks and national certifications will go a long way to strengthening CHW programs, not least because money flows to where political will is. For now, these initiatives are mostly donor-funded, and too often project- or disease-based. Part of governments' work ahead will be to find innovative ways to sustainably finance the health sector as a whole and strengthen health system foundations, including community-led systems and responses. Through its advocacy strategy, Africa CDC intends to advocate for increased and coordinated domestic and external investment in community health systems.
We must match CHWs’ incalculable contribution with investments in their full potential with leadership and resources.
When asked during a recent webinar about what motivates volunteer CHWs, Prossie Muyingo, a CHW in Uganda, said: “You can’t just sit when your baby’s dying, even if it’s not in your house.”
Policymakers must do justice to the dedication, resilience, and resolve CHWs display to reach everyone, everywhere with quality health services — for everyone’s sake. We should believe Prossie and her fellow CHWs when they say they will carry us to universal health coverage, and give them the tools to facilitate their success.
About the Authors
Mohammed Abdulaziz is Head, Division of Disease Control and Prevention, Africa CDC
Maziko Matemba is community health ambassador, Ministry of Health and Population, Malawi
Herilinda Temba is PACT CHW lead and principal technical officer, Division of Disease Control and Prevention, Africa CDC
John Wanyungu is deputy head, Division of Community Health Services in Kenya’s Ministry of Health
Photo credit: Living Goods
Category: Civil society and communities
